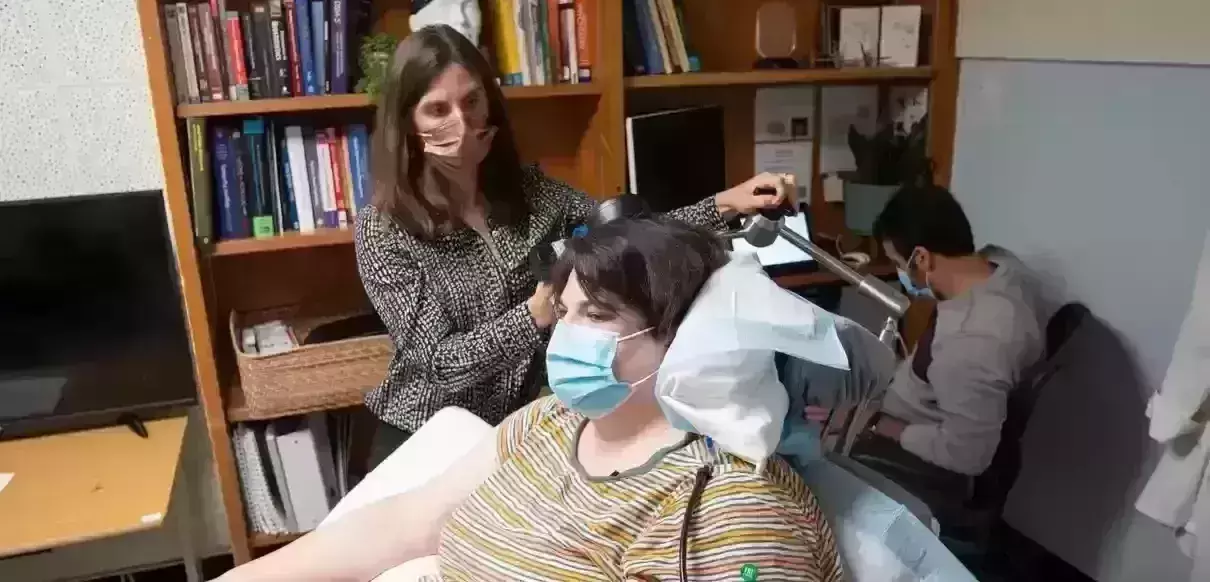
Electrical brain implant relieves woman's severe depression in US
text_fieldsIn a "stunning" advance that offers hope to those diagnosed with intractable mental illnesses, a woman with severe depression has been successfully treated with an experimental brain implant.
The cutting edge device works by detecting patterns of brain activity linked to depression and automatically interrupting them using tiny pulses of electrical stimulation delivered deep inside the brain.
Andrew Krystal, co-senior author on the new study explained that the new study points the way to a new paradigm that is desperately needed in psychiatry.
As per a report by The Guardian, the researchers developed a precision-medicine approach that has successfully managed the patient's treatment-resistant depression by identifying and modulating the circuit in her brain that's uniquely associated with her symptoms.
The 36-year-old patient, Sarah is now elated as the therapy has now allowed her to laugh spontaneously for the first time in five years.
"When I first received stimulation I felt the most intensely joyous sensation and my depression was a distant nightmare for a moment," said Sarah. "I just laughed out loud. It's the first time I had spontaneously laughed or smiled … in five years."
The success of this cutting edge approach in the field of psychiatry is now hailed as hugely significant although the therapy has been tested in only one patient – and would only ever be suitable for those with severe illness.
It is the first demonstration that the brain activity underlying the symptoms of mental illness can be reliably detected and reveals that these brain circuits can be nudged back into a healthy state, even in a patient who has been unwell for years.
Katherine Scangos, an assistant professor of clinical psychiatry at the University of California, San Francisco (UCSF), who led the work remarked that they haven't been able to do this kind of personalised therapy previously in psychiatry.
"This success in itself is an incredible advancement in our knowledge of the brain function that underlies mental illness," Scangos said.
The deep brain stimulation (DBS) approach has been used to treat tens of thousands of patients with Parkinson's disease and epilepsy over the past two decades.
However, several trials for depression have ended in disappointment.
A major challenge was that the brain does not appear to have a single "depression area" with several interconnected areas in play and these can differ between people.
Prof Edward Chang of the University of California San Francisco, the neurosurgeon who treated Sarah stated that the study has helped them to start recognizing some of the complexity involved in how mood is regulated in the brain as a network.
A meticulous, personalised approach paved the way for the latest advance. In an initial phase lasting a week, a temporary brain implant recorded a wide range of activity while Sarah regularly logged her mood on a tablet. A machine-learning algorithm was used to identify a telltale pattern of activity in the amygdala region accompanying Sarah's lowest points.
In the second round of minimally invasive surgery, a permanent device was implanted, with a tiny battery unit embedded in her skull, to detect the "depression signature" activity in the amygdala and automatically deliver stimulation to the ventral striatum.
This happens about 300 times each day, equivalent to about 30 minutes of stimulation. The electrical pulse is not accompanied by any sensation, Sarah said, aside from a subtle feeling of alertness and positivity.
The device costs about $35,000 (£26,000) and is an adapted version of one normally used to treat epilepsy, called the NeuroPace RNS System. The UCSF team has already enrolled two more patients and hopes to recruit a further nine to assess whether the technique can be more widely applied.